Last week I had the privilege of visiting some clinics in a remote part of Gorkha district in Nepal and that trip got me reflecting on different styles of medical practise. I've posted some photos on Instagram @wilson.howarth and I shall write about my recent experience soon but meanwhile here are some notes about the mission to Nigeria I went on in the summer.
Early July, a message with the title ‘Mad idea’ arrived in my inbox. Intrigued, I opened it immediately. It was an invitation to go to Nigeria for three weeks ‘as soon as possible’. Then over the next several days I discovered that this voluntary assignment was to investigate a malaria outbreak. I said I was interested, but then had my usual doubts about my competence. Yes, as a doctor with an interest in tropical medicine, I knew a bit about malaria but I’d never personally diagnosed a case – except in bats. I knew a lot about
Anopheles mosquitoes but that wasn’t likely to be relevant in understanding what seemed to be a new outbreak. I’d run health sessions for this NGO’s volunteers over many years but I didn’t know Africa. I’d never been to West Africa and I had absolutely no experience of treating malaria. What use would I be then?
My link person within the NGO had more confidence in my abilities and joked that my one key qualification was ‘understanding the demographic’. I was to be investigating volunteers aged 18 – 25 and I had one of those at home. I have more letters after my name than in it but she knew that I understood how likely it was that the volunteers would follow advice, take their malaria pills and protect themselves from bites.
I’ve already written a little about the trip and my homestay in previous blogs (the first is
Short trip to Nigeria then
Nigerian Swallow) and thought I’d now detail my unusual mission to Nigeria. The volunteers were based in a small town where electricity was at best intermittent and facilities were basic. They slept under insecticide-impregnated mosquito nets and seemed to understand and comply with malaria avoidance strategies. Why then had eight of them been treated for malaria 12 times in the previous six weeks? Could this be a new malignant strain of malaria that was resistant to antimalarial pills? Was it another infection altogether?
For some of the British volunteers this was their first experience of living in a low-income setting and several were understandably spooked when they became unwell – especially as I’d hammered home my message at the pre-departure health briefings that malaria is a killer. They may also have been aware that Lassa Fever was taking lives not many miles away. Local doctors also reported treating lots of people for typhoid, which is another dangerous disease.
I spent lots of time talking to the volunteers. They were well supported by their NGO and could readily pitch up at the local private hospital if they felt unwell. I took a retrospective clinical history about how each volunteer had felt in the days leading up to each malaria diagnosis, and strangely only one told a tale that suggested she’d had the high fever typical of malaria, and she’d clearly had suffered an attack of bacilliary dysentery.
I questioned various local staff and doctors. I visited the medical laboratories where malaria is diagnosed. I tested the volunteers using two different kinds of Rapid Diagnostic Kits.
None of them had had malaria.
This was a welcome surprise but what was going on?
Doctors in different countries practise different styles of medicine. The local tendency was a scattergun approach – prescribing a range of medicines that would cure all the nastiest diseases, including typhoid, dysentery and malaria. In regions where patients may not return to the doctor if their symptoms don’t improve, this strategy probably saves lives.
The local doctors were over-prescribing but had done no harm. I could reassure the volunteers. My final challenge though was to explain that although none of the volunteers had suffered malaria, they could still have confidence in their doctors and accept that taking five or six or even nine prescriptions was acceptable even where one would have been enough.
Thus I could leave Nigeria confident that the volunteers were not all about to be wiped out by an invincible mutant parasite.
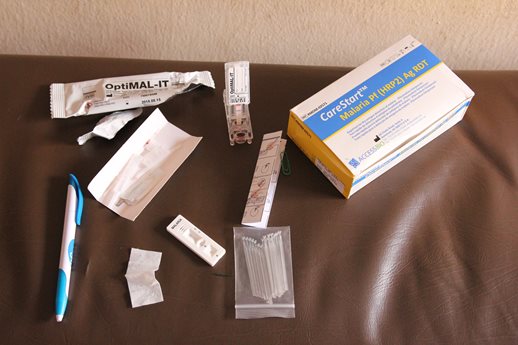 |
| Two brands of Rapid Diagnostic blood-Testing kits for malaria |
There's more about my Nigeria trip here too:
Nigerian serenade,
Fake news? and
Priorities